views
Obesity is a medical condition in which excess body fat has accumulated to the extent that it may have a negative effect on health, leading to reduced life expectancy and/or increased health problems.
Obesity is defined by body mass index (BMI)
BMI is calculated by using the following formula:
BMI = Weight (in KG) / height (m) x height (m)
Genetics affect hormones involved in fat regulation. A person is more likely to develop obesity if one or both parents are obese.
If one is eating more calories than the body is using, one will store these extra calories as fat and gain weight.
Improved transportation facilities, mechanisation of jobs and leisure activities centred around TV/Computers lead to little/no physical activity.
Easily available processed, calorie dense, unhealthy foods and oversized food portions increase the chances of becoming obese.
The reason for the weight gain with the medications differs for each medication. Medications associated with weight gain include certain anti-depressants, anti-convulsants, diabetes medications, certain hormones like steroids, some high blood pressure medications and antihistamines.
Some psychological factors like emotional stress, anger, sadness etc. can also lead to weight gain, as people tend to eat more during such conditions.
Such as hypothyroidism, insulin resistance, polycystic ovary syndrome, and cushing’s syndrome also contribute to obesity.
Morbid obesity us a state of severe obesity defined by following BMI Criteria :
Those who are morbidly obese are at greater risk for illness including diabetes, high blood pressure, sleep apnea, gastro esophageal reflux disease (GERD), gallstones, osteoarthritis, heart disease, infertility and increased chances of cancer. Morbid obesity can also be the cause of many psychological disorders like anxiety, depression, marital disharmony, poor body image at social and work places etc.
Morbid obesity is an extreme health hazard with medical, psychological, social, physical and economic comorbidities.
The various treatment options available for obesity are as follows :
For people with BMI less than 32.5 kg/m2, who do not qualify for weight loss surgery, we offer a weight management programme under the guidance of a bariatric physician, nutritionist and psychologist.
Indians are genetically susceptible to weight accumulation, especially around the waist. An obese individual is much more susceptible to diseases like diabetes, hypertension, osteoarthritis and obstructive sleep apnea.
Studies have shown that, in males, compared with a healthy weight man, an obese man is 5 times more likely to develop type 2 diabetes. Whereas in females, an obese woman, compared with a healthy weight woman is almost 13 times more likely to develop type 2 diabetes.
The traditional approach to treat type 2 DM has been step wise introduction of lifestyle changes with or without oral medications, saving the insulin therapy for last. Treatment should focus equally on remission of both diabetes and obesity and needs to be widely understood. In the light of the escalating global diabetes crisis, the need of the hour is to identify interventions that provide a long term metabolic outcome (obesity and associated diseases remission).
There are several methods of treating obesity, such as lifestyle changes encompassing behaviour modification, physical activity, diet modification and medical management. It has been seen that the sustained weight loss is achieved by only 10% of the population.
Bariatric Surgery (obesity surgery) is the most effective long-term treatment for obesity with the greatest chances for amelioration and even resolution of obesity-associated diseases.
In the given scenario of increasing morbidity and mortality due to type II diabetes mellitus and obesity, bariatric surgery has emerged as a promising treatment. It provides exceptional sustained weight loss and remission of type II diabetes in addition to improvement in the other co-morbidities and quality of life.
Bariatric/obesity/weight loss surgery is a treatment option for patients suffering with morbid obesity. It is considered to be the most effective treatment for obesity in terms of maintenance of long term weight loss. Moreover, it causes significant improvement in obesity-related co-morbid conditions like type 2 diabetes, high blood pressure, joint pains, sleeping disorders like sleep apnea, heart diseases, infertility issues and more.
Bariatric surgery is performed using laparoscopic technique (keyhole surgery – minimally invasive) and most of the patients are walking around on the same day of the surgery.
Bariatric surgical procedures cause weight loss by restricting the amount of food the stomach can hold, causing less absorption of food, or by a combination of both gastric restriction and less absorption. The weight loss surgeries are performed using minimally invasive techniques (Laparoscopic surgery causes significantly less pain and early recovery. The cosmetic outcomes are excellent).
Common Bariatric Surgery options which are available:
One qualifies for bariatric surgery if the following criteria are met:
Choice of the surgical procedure which is best suited to patient depends on:
Gastric bypass surgery is the most time honoured bariatric procedures that dates back to 1960’s. The long term outcome of this procedure are well researched and documented and today it is one of the most common and successful weight loss procedures. It is called as 'The Roux-en-Y Gastric Bypass (RYGB)’ and is considered as the ‘gold standard’ of weight loss surgery. It should not be confused with other types of bypasses.
The gastric bypass works by creating a small stomach pouch which restricts intake of food and facilitates significantly smaller meals, which translates into less calories consumed. A major portion of the stomach and a part of the small intestine is bypassed (i.e. food does not enter this portion) which causes less absorption of food thus leading to lesser absorption.
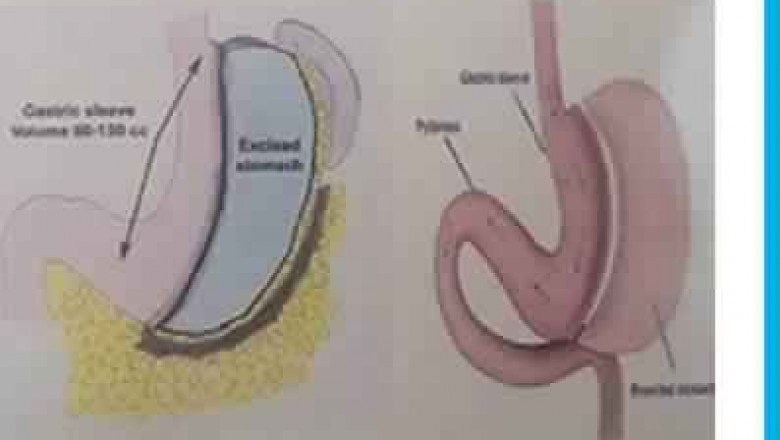
This surgery is performed by removing approximately 80% of the stomach. The remaining stomach looks like a banana or a sleeve of a shirt and hence called as ‘sleeve’.
The new stomach pouch being much smaller restricts food intake thus leading to weight loss.
In the long run (few years after the surgery), Vitamin B12 and some other nutrient deficiencies are observed. However, most of them can be managed effectively by treating team. Regular follow up with the team and compliance with instructions is strongly recommended. It has been proved that follow ups ensure excellent outcomes and prevent adverse events.
Generally, hospital stay can be between three to four nights, unless there are situations demanding longer stay due to co morbid conditions/high risk patients/ adverse events.
It will depend on the type of surgery and type of your work. In general, plan to take about 7-10 days off from work in usual cases where recovery is uneventful.
Yes, regular exercise is important for maintaining weight loss.
Yes, you need to take long term supplements like vitamins, calcium, iron (which of course is better than the medications needed for various diseases that are associated with obesity like diabetes, high blood pressure, high cholesterol and more).
Care for morbidly obese patients requires a comprehensive and multi disciplinary set up comprising of bariatric surgeon, bariatric anaesthetist, bariatric physician, bariatric nutritionist, bariatric coordinator, psychologist, endocrinologist and physiotherapist.
Obesity and weight loss issues are complex and difficult to handle alone. At Max Institute of Minimal Access Metabolic & Bariatric, we offer regular support group meetings – to all those who have undergone bariatric surgery and those who are considering it.
These meetings are our attempt to re-emphasize on the fact that the operated patients are not alone in this journey. Attending a support group proves to be a very empowering experience and great opportunity to interact with others going through same phase.
Unlike traditional support groups, we provide a very interactive and informative program. Every session is based on a theme such as, tips for successful weight loss, tips on how to eat out healthy, importance of exercises, nutrition, impact on body image and mental health. We believe that family involvement is imperative for all operated patients and we welcome all who are keen to attend the meetings.
These regular meetings offer support and motivation to the operated patients for all their physical issues. We have seen patients speaking their hearts out in these meetings about the apprehensions they carried before undergoing the surgery and how the surgery might change their life. Post surgery, these patients are amazed by the transformation they witness in themselves. These meetings prove to be an excellent platform for patients to get together, listen to other people’s experiences after the surgery and open up. Few months after surgery, all that these patients need is a little motivation. These meetings provide a much needed boost which encourages these patients to maintain a healthy lifestyle.
To enjoy good health, to bring true happiness to one's family, to bring peace to all, one must first discipline and control one's own mind. If a man can control his mind he can find the way to Enlightenment.












